Abstract
Case Study
Ms. S.G., a 56-year-old woman with a poorly differentiated squamous cell carcinoma of the anal canal, American Joint Committee on Cancer stage III (T2, N1, M0), was initially diagnosed in December, 2007 at an outside institution after she had noted blood in her stool for approximately 6 months. Her medical history was unremarkable. She had no known history of HIV or other sexually transmitted diseases. At the time of presentation, Ms. S.G. had an Eastern Cooperative Oncology Group performance status of 1 related to cancer-related pain. Her appetite and weight were both stable.
A complete colonoscopy demonstrated a large, immobile, ulcerated, firm, 4-cm lesion in the distal rectum, arising from the anal canal. Initial staging positron emission tomography/computed tomography (PET/CT) scan revealed a hypermetabolic inferior anorectal mass with left perirectal and presacral nodal metastases. There was no definite evidence of distant metastatic disease.
Ms. S.G. received chemoradiation treatment following her diagnostic studies, with a total dose of 45 Gy over 26 fractions to the pelvis with concurrent infusional fluorouracil (5-FU; 2, 450 mg over 7 days) and mitomycin C (12 mg/m2 on day 1) at an outside institution. However, during her chemoradiation therapy, Ms. S.G. experienced a 3-week treatment break due to severe radiation dermatitis, as recommended by her outside treating oncologist.
Upon treatment completion, Ms. S.G. underwent a biopsy of the anal canal, which revealed no evidence of residual malignancy. As recommended by her treating oncologist, she received four additional cycles of adjuvant infusional 5-FU in combination with leucovorin. Shortly thereafter, Ms. S.G. developed progressive pelvic pain. She underwent a second PET/CT scan, revealing mixed findings: interval resolution of abnormal standardized uptake value (SUV) activity at the primary tumor in the anal canal, but an increase in the size and SUV of nodal disease within the left perirectal and presacral regions. A CT-guided biopsy noted a perirectal abscess requiring drainage but was inconclusive for disease recurrence; Ms. S.G. was treated with IV antibiotics.
Six weeks later, repeat radiographic imaging noted additional changes suspicious for regional recurrence, which was biopsy-confirmed. Ms. S.G. was subsequently referred to MD Anderson Cancer Center for consideration of salvage pelvic exenteration.
On physical exam a mass was palpated in the left lower quadrant, but there was no evidence of inguinal adenopathy. On digital rectal exam there was notable external erythema with a fixed mass and moderate sphincter tone. A chest CT scan showed no definite evidence of metastatic disease, but an MRI of the abdomen/pelvis indicated the presence of a complex partially necrotic mass (7.6 × 4.9 × 7.3 cm3) extending to the rectosigmoid junction, inseparable from the left lateral bowel wall, with partial encasement of the bowel. In addition, there was infiltration of the left piriformis muscle and cervix consistent with local recurrence. She was referred to medical oncology and radiation oncology for consideration of reirradiation with concurrent neoadjuvant chemotherapy for palliation and possible surgical resection.
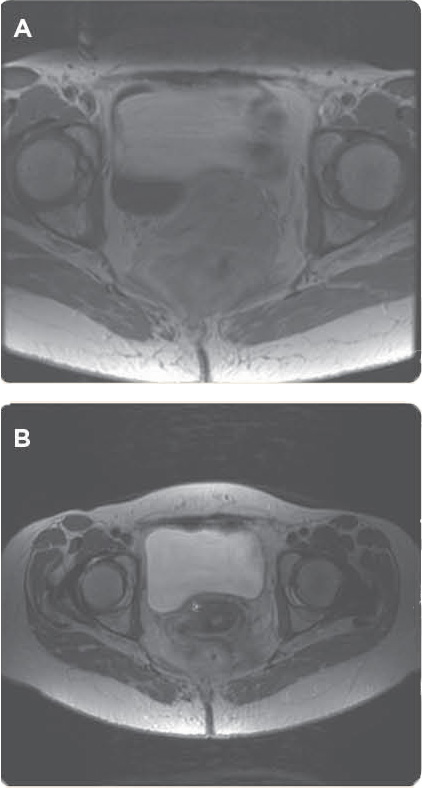
In early December 2008, Ms. S.G. received intensity-modulated radiation therapy (IMRT), with a total dose of 27 Gy over 18 fractions. She received concurrent infusional 5-FU at 300 mg/m2/day, from Monday to Friday, on the days of radiation. She also received a weekly bolus dose of cisplatin at 20 mg/m2. The intent was to treat to 30 Gy, but the patient deferred further treatment early due to anorectal irritation. She then underwent restaging with a PET/CT scan and a pelvic MRI in February 2009, revealing radiographic partial response of the known pelvic recurrence and reduced pelvic pain (Figures 1A and 1B).
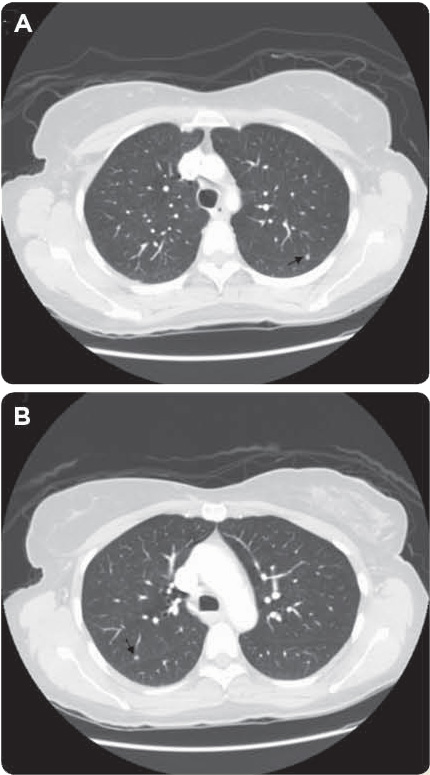
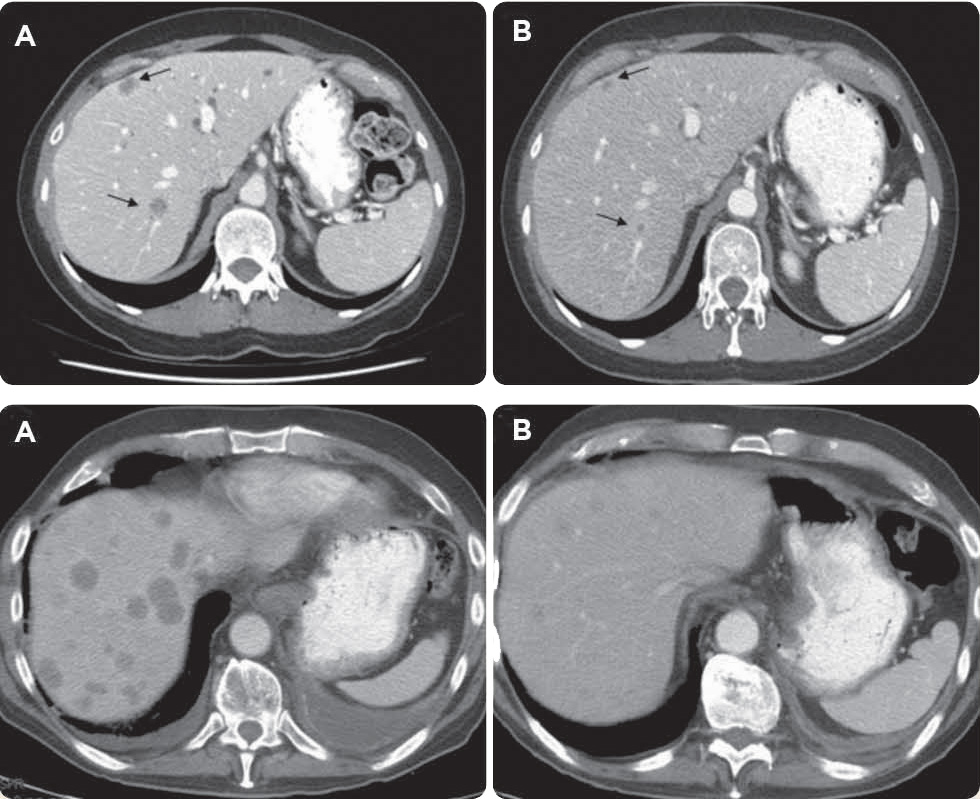
Unfortunately, in the interim, she developed multiple bilateral liver lesions and punctate pulmonary nodules consistent with distant disease (Figures 2A, 2B, and 3A).
Ms. S.G. proceeded to undergo systemic chemotherapy with carboplatin at an area under the concentration-time curve of 5 and paclitaxel at 175 mg/m2 day 1, every 21 days. She tolerated the treatment well. After three cycles of chemotherapy, radiographic imaging indicated a mixed response to treatment: interval resolution of the pulmonary nodules, stability of disease in the pelvic mass, but progression of the hepatic metastases.
Given Ms. S.G.'s continuing excellent performance status, further treatment was recommended. Based on recent published literature, a regimen of cisplatin at 80 mg/m2 day 1, vinorelbine at 25 mg/m2 day 1 (repeated every 28 days), and weekly cetuximab (VCC) at 250 mg/m2 was initiated. Remarkably, following three cycles of treatment, despite receiving multiple prior lines of chemotherapy, her restaging CT scan demonstrated complete radiographic response of the intrathoracic disease, stable response of the anorectal mass, and near-complete resolution of the hepatic lesions (Figures 3A and 3B).
Overall, Ms. S.G. had tolerated her treatment very well. Given her response and tolerability, she was evaluated again for curative surgical resection. However, she opted to receive the VCC regimen closer to home and was lost to follow-up. Unfortunately, we were unable to obtain medical records confirming if she indeed received additional treatment as recommended. Ms. S.G. was noted to have passed away due to progression of her disease approximately 6 months later.